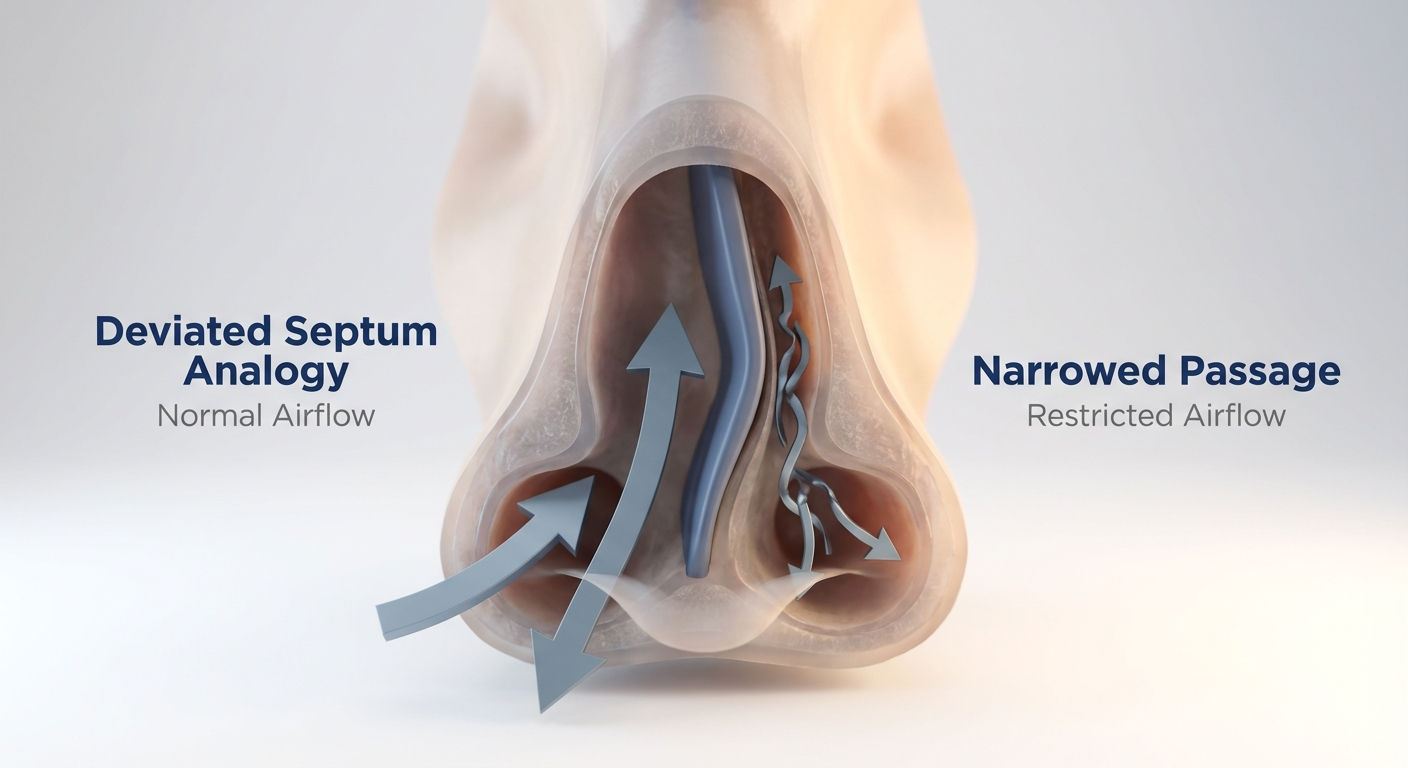
The Link Between Nasal Obstruction and Chronic Sinusitis
Why a “Stuffy Nose” Can Be More Than a Nuisance
Many people live with a “stuffy nose” for months and assume it’s just allergies, weather changes, or a lingering cold. But when nasal blockage becomes persistent—or keeps coming back—it may be connected to chronic sinusitis (also called chronic rhinosinusitis).
What’s important (and often surprising) is that the link between nasal obstruction and chronic sinusitis can be bidirectional:
- Nasal obstruction may make it harder for the sinuses to ventilate and drain normally.
- Chronic sinus inflammation can also cause swelling and congestion that worsens obstruction.
Note: “Sinusitis” can refer to both acute infections and chronic inflammatory conditions. This article focuses on chronic rhinosinusitis, a long-term, often inflammatory condition.
Nasal blockage is also one of the hallmark symptoms people report with chronic sinusitis, along with drainage issues and facial pressure (Mayo Clinic). A common real-life pattern is: symptoms ease a bit with sprays or rinses, then flare again at night, during travel, or with seasonal changes. If that cycle sounds familiar, it’s worth looking at both inflammation and anatomy—because they often interact.
The link can be bidirectional, but that doesn’t mean every case of obstruction causes sinusitis or vice versa. Each person’s situation is unique.
A brief note on self-diagnosis: because many nasal and sinus symptoms overlap with other conditions, a professional evaluation helps ensure the right diagnosis and a tailored plan.
Bottom line: persistent “stuffy nose” isn’t always simple—especially when inflammation and anatomy reinforce each other.
Quick Definitions (So the Rest Makes Sense)
What is nasal obstruction?
Nasal obstruction is the sensation that air can’t move through the nose normally. It can be constant or come and go, and it may alternate from one side to the other.
Common ways people describe it include:
- “I can’t breathe through my nose.”
- “My nose blocks at night.”
- “One nostril always feels closed.”
Think of the nose like a two-lane road. Inflammation is like temporary construction narrowing the lanes; a structural issue is like the road being built narrower in the first place. Either way, airflow slows—especially when both happen together. Identifying whether inflammation, anatomy, or both are driving the problem helps guide treatment.

What is chronic sinusitis (chronic rhinosinusitis)?
Chronic sinusitis/chronic rhinosinusitis is long-lasting inflammation of the nasal and sinus lining that can affect breathing, smell, mucus drainage, and facial comfort/pressure. Nasal obstruction is a primary symptom (Mayo Clinic). Research describes chronic rhinosinusitis as a complex inflammatory condition with multiple contributing factors (PMC).
Some people expect sinusitis to feel like a constant “infection,” but chronic rhinosinusitis often behaves more like an ongoing inflammatory condition—where symptoms can wax and wane instead of staying severe every day.
Key idea: chronic rhinosinusitis is typically inflammatory and multifactorial, not just a lingering infection.
How Nasal Obstruction Can Contribute to Chronic Sinusitis
Obstruction can interfere with airflow and mucus drainage
Your sinuses are air-filled spaces that rely on small natural openings to ventilate and drain mucus. When the nasal lining is swollen—or when the passage is physically narrowed—mucus drainage may become less efficient.
A simplified version of the cycle:
1) Narrowing/swelling reduces airflow and drainage
2) Mucus can thicken or pool
3) Irritation and inflammation may increase
4) Symptoms persist or recur
A helpful analogy: a sink with a partially clogged drain still works, but it drains slowly—so buildup is more likely and harder to “reset” to normal (Mayo Clinic).
When drainage pathways stay narrowed, it’s harder to break the cycle—even with otherwise good care.

Structural narrowing raises risk for “getting stuck in the cycle”
Some causes of nasal blockage are structural (anatomic), meaning the space is physically tighter than it should be. Common contributors include:
- Deviated septum
- Nasal polyps
- Enlarged turbinates (tissue along the sidewalls that can swell)
These issues can narrow airflow, contribute to turbulence, and potentially reduce effective sinus ventilation and drainage—especially when inflammation is also present. If the baseline nasal airway is narrow, even a small amount of swelling (from allergies, irritants, or viral illness) can cause a disproportionately big jump in symptoms. For a deeper dive on one common structural issue, see how a deviated septum affects sinus infections.
If your airway starts narrow, small flares of swelling can feel like big problems.
What the evidence says (and what it doesn’t)
Chronic rhinosinusitis is often multifactorial. Research supports an association between certain nasal obstructions and chronic rhinosinusitis, but the overall cause-and-effect story can be complex—because anatomy, inflammation, allergies, environment, and immune responses can overlap (PubMed). A clinician might say: “We’re usually treating a combination of swelling and airflow mechanics—so the plan has to match what we find on exam and imaging.”
Association is real for many patients, but one root cause rarely tells the whole story.
How Chronic Sinusitis Can Cause (or Worsen) Nasal Obstruction
Inflammation and swelling narrow the nasal passages
Even without a major structural problem, chronic inflammation can lead to persistent swelling of the nasal lining. That swelling alone can create the ongoing “blocked nose” sensation many people describe (Mayo Clinic). People often notice this most at night; mouth-breathing may worsen dry throat, snoring, and sleep disruption.
Inflammation alone can make the nose feel closed, especially at night.

Polyps and thickened tissue can develop over time
In some people, long-standing inflammation is associated with nasal polyps—soft, noncancerous growths that can physically block airflow and interfere with drainage (Mayo Clinic). When present, polyps add mechanical blockage on top of inflammation.
When polyps join inflammation, obstruction often feels more persistent.
Signs You Might Be Dealing With More Than Temporary Congestion
Symptoms commonly seen with chronic sinusitis + obstruction
If symptoms last for weeks to months, occur frequently, or affect daily life, it may be more than a passing cold. Common symptoms include:
- Nasal blockage/congestion
- Facial pressure/fullness
- Thick drainage or postnasal drip
- Reduced sense of smell
- Fatigue and sleep disruption (Mayo Clinic)
A practical clue: if you’re saying, “I don’t remember the last time I breathed clearly through my nose,” it may be time to get evaluated rather than continuing to power through.
When to see an ENT (red flags and timing)
Consider an ENT evaluation if:
- Symptoms persist despite appropriate home care and over-the-counter measures
- Symptoms keep recurring
- You have ongoing one-sided obstruction (often needs a closer look)
Seek urgent evaluation for severe facial swelling, high fever, vision changes, or severe headache.
For next steps, see deviated septum and chronic nasal congestion—what to do next.
If symptoms are persistent, recurring, or one-sided, get a focused evaluation.
What Causes Nasal Obstruction? (Common Buckets)
Inflammatory causes
Inflammation can narrow the nasal lining and increase mucus production. Common inflammatory causes include:
- Allergic rhinitis
- Non-allergic rhinitis
- Chronic sinus inflammation (Mayo Clinic)
Many people have a mix of triggers—for example, allergies plus sensitivity to smoke, fragrances, or temperature shifts.
Structural causes
Structural causes are physical/anatomic issues that limit space, such as:
- Deviated septum
- Turbinate hypertrophy (enlarged turbinates)
- Nasal valve narrowing (Kaplan Sinus Relief; Sinusitis Treatment NYC)
These are often missed without a focused nasal exam.
Growths and other contributors
- Nasal polyps are a common growth-related cause of obstruction in chronic inflammation (Mayo Clinic).
- Less commonly, other masses can contribute—another reason persistent symptoms deserve evaluation.
Inflammation, structure, and growths can coexist, so a thorough exam matters.
How Clinicians Figure Out What’s Driving Your Symptoms
History + nasal exam
A clinician typically starts with a symptom history:
- Seasonal vs. year-round
- One-sided vs. both sides
- Nighttime patterns and sleep impact
- Triggers (smoke, irritants, workplace exposures)
A focused nasal exam helps identify signs of swelling, drainage, septal deviation, or suspected polyps. Bring notes on when symptoms started, what helps/worsens them, and what you’ve tried (sprays, rinses, allergy meds).
Nasal endoscopy and/or CT imaging (when appropriate)
When symptoms are persistent, recurring, or unclear, an ENT may recommend nasal endoscopy and/or CT imaging to assess:
- Septal deviation and narrowing patterns
- Polyps
- Areas of sinus blockage
- Inflammation patterns (Mayo Clinic)
Imaging complements symptoms by showing what’s physically happening in the nose and sinuses.
A good plan matches what you feel with what’s seen on exam and imaging.
Treatment Options That Target Both Obstruction and Sinusitis
Home and lifestyle supports (adjuncts)
These don’t cure chronic rhinosinusitis, but they can support comfort and mucus movement:
- Saline rinses/irrigation
- Managing indoor humidity
- Avoiding smoke and irritants
- Sleep positioning (some people notice less nighttime blockage with head elevation)
Consistency often matters more than intensity.
Medical therapies (often first-line)
Many people start with medical management, which may include:
- Nasal steroid sprays
- Allergy evaluation/management when relevant
- Other clinician-directed therapies
Because chronic rhinosinusitis often involves inflammation rather than bacterial infection, antibiotics are generally reserved for acute bacterial exacerbations—not as a universal fix for chronic symptoms (Mayo Clinic).
When structural obstruction is a major driver: procedural options
If a clearly documented structural issue (such as a deviated septum) is a major contributor to obstruction, addressing anatomy may help reduce the ongoing “obstruction–inflammation” loop for selected patients. Learn more about the role of septoplasty in treating chronic sinusitis.
For many, the best results come from treating both inflammation and structure.

Spotlight: Septoplasty and Minimally Invasive Balloon-Assisted Approaches
This section is educational and not a promise of results. Treatment choices depend on individual anatomy, symptoms, and clinician evaluation.
Why correcting a deviated septum may help some chronic sinusitis patients
If septal deviation significantly limits airflow, improving nasal patency may:
- Make nasal breathing easier
- Support more normal airflow patterns
- Potentially help drainage pathways function more effectively
This targets one part of the link between nasal obstruction and chronic sinusitis: persistent mechanical narrowing. Individual experiences vary.
Balloon-assisted endoscopic septoplasty (ClearPath Nasal Balloon)—what “minimally invasive” can mean
Balloon-assisted septoplasty uses controlled balloon pressure under endoscopic visualization to help mobilize and reposition portions of the septum. In selected cases, a balloon-assisted approach may reduce the need for more extensive tissue lifting and associated steps. For an explainer, see what is balloon septoplasty?
Not all septal deviations are suitable for balloon-assisted treatment; careful patient selection is important.
Early clinical outcomes reported for the ClearPath Nasal Balloon (CNB)
In an early retrospective analysis of this technique and device, reported findings included:
- Safety profile: In 107 cases, no major complications were observed (no septal perforation, hematoma, mucosal injury, or synechia).
- Imaging improvements: In 23 patients with pre/post CT scans, septal alignment improved by 45% at the point of maximal deviation and 22% at the nasolacrimal duct (p = 0.005).
- Symptom improvement: Average SNOT-22 decreased by 24%, with notable improvements in congestion, facial pressure/headache, and sleep quality at 1 month.
- Procedure efficiency concept: Reduced need for flap elevation, suturing, and packing may streamline the procedure and potentially reduce anesthesia time (which varies by patient and setting).
While these results are encouraging, they reflect preliminary, retrospective data; outcomes vary, and all procedures carry risks. Discuss potential benefits and risks with your surgeon.
Who might be a candidate (and who might not)
Potential candidates may include people with:
- Documented septal deviation
- Persistent obstruction despite appropriate medical therapy
- Symptoms that affect sleep, exercise, or quality of life
Not everyone with chronic rhinosinusitis has a structural blockage, and not everyone needs a procedure. Many people require a plan that addresses both inflammation and anatomy.
Ask your ENT to review your exam and imaging with you—and to explain why a given approach fits your anatomy and goals.
FAQs (Patient-Friendly)
Can a deviated septum cause chronic sinusitis? A deviated septum can contribute for some people by narrowing airflow and potentially affecting drainage. But chronic rhinosinusitis is often multifactorial, so a deviated septum isn’t always the only driver (Mayo Clinic; PubMed).
If I fix my obstruction, will my sinusitis go away? Improving obstruction can help some patients—especially if a structural problem is a major contributor. Long-term results also depend on inflammation control, allergies, polyps, irritant exposure, and consistent medical care.
What’s the difference between treating inflammation vs treating structure?
- Inflammation-focused treatment aims to reduce swelling and mucus issues (for example, sprays, irrigation, allergy management).
- Structure-focused treatment aims to widen airflow pathways (for example, septoplasty, turbinate reduction, and polyp management when indicated).
Think “both-and,” not “either-or,” when symptoms are driven by mixed factors.
Key Takeaways (Summary)
- The link between nasal obstruction and chronic sinusitis is often two-way: obstruction can worsen sinus issues, and chronic sinus inflammation can worsen obstruction.
- Structural issues like deviated septum, nasal polyps, and enlarged turbinates can add a mechanical component to congestion and drainage problems.
- Chronic rhinosinusitis is complex—association doesn’t always mean one single cause.
- If symptoms persist or recur, an ENT evaluation can clarify whether inflammation, anatomy, or both are driving the problem.
A tailored plan—grounded in exam and imaging—often works best.
Next Steps
If you’re noticing ongoing congestion, consider:
- Tracking symptoms (nighttime blockage, facial pressure, smell changes, triggers)
- Scheduling an evaluation if symptoms last for weeks/months or keep coming back
- Asking whether structural obstruction is part of your overall picture—and what options best fit your goals
If you’ve been told you have a deviated septum (or suspect one), you can also ask your local ENT about both traditional septoplasty and minimally invasive alternatives—including ClearPath Nasal Balloon–assisted approaches—so you understand the full range of options.
The sooner you match treatment to the true drivers of your symptoms, the sooner you can break the cycle.
References
- Mayo Clinic. Chronic sinusitis—Symptoms and causes. https://www.mayoclinic.org/diseases-conditions/chronic-sinusitis/symptoms-causes/syc-20351661
- PMC (PubMed Central) article on chronic rhinosinusitis. https://pmc.ncbi.nlm.nih.gov/articles/PMC12644427/
- PubMed record (association/complexity). https://pubmed.ncbi.nlm.nih.gov/39271710/
- Kaplan Sinus Relief (nasal obstructions overview). https://www.kaplansinusrelief.com/blog/nasal-obstructions-how-to-treat/
- Sinusitis Treatment NYC (causes of nasal obstruction). https://www.sinusitistreatmentnyc.com/blog/top-causes-of-nasal-obstruction-understanding-and-treating-your-symptoms/
- Zadeh MD (chronic nasal obstruction causes/treatments). https://www.zadehmd.com/post/what-causes-chronic-nasal-obstruction-and-how-to-treat-it
- Dillard JD, Koudouovoh C, Lee V, et al. Outcomes of force-directed balloon-assisted endoscopic septoplasty: a retrospective analysis with a new technique and device. Rhinology Online. 2026;9:18–23. http://doi.org/10.4193/RHINOL/25.018
Disclaimer
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Resent posts
Contact us
Have questions about the ClearPath Nasal Balloon System? Our team is here to help with product inquiries, demonstrations, or order support.



.webp)