Nasal Obstruction: It’s More Than Just a Stuffy Nose
If you’ve ever thought, “I can’t breathe through my nose,” it’s easy to chalk it up to a cold, seasonal allergies, or a passing bout of congestion. But for many people, that “blocked nose” feeling is a sign of something more persistent—sometimes structural, sometimes inflammatory, and often a mix of both.
That matters because breathing well through your nose isn’t only about comfort. Ongoing symptoms can affect sleep and nasal breathing, energy, focus, and even mood. And it’s common: estimates suggest chronic or persistent nasal congestion/obstruction affects about 12% of the U.S. population.¹
This guide breaks down what nasal obstruction really is, why it can become chronic, how ENTs evaluate it, and what treatments—medical and procedural—can help.
What Is Nasal Obstruction (and How Is It Different From a Normal Stuffy Nose)?
A simple definition patients can recognize
Nasal obstruction means reduced airflow through the nasal passages. It may be persistent, recurring, or mainly affect one side. People often describe it as:
• A constant feeling of blockage
• “Not enough air” through the nose
• Mouth breathing (especially at night)
• Reduced exercise tolerance²
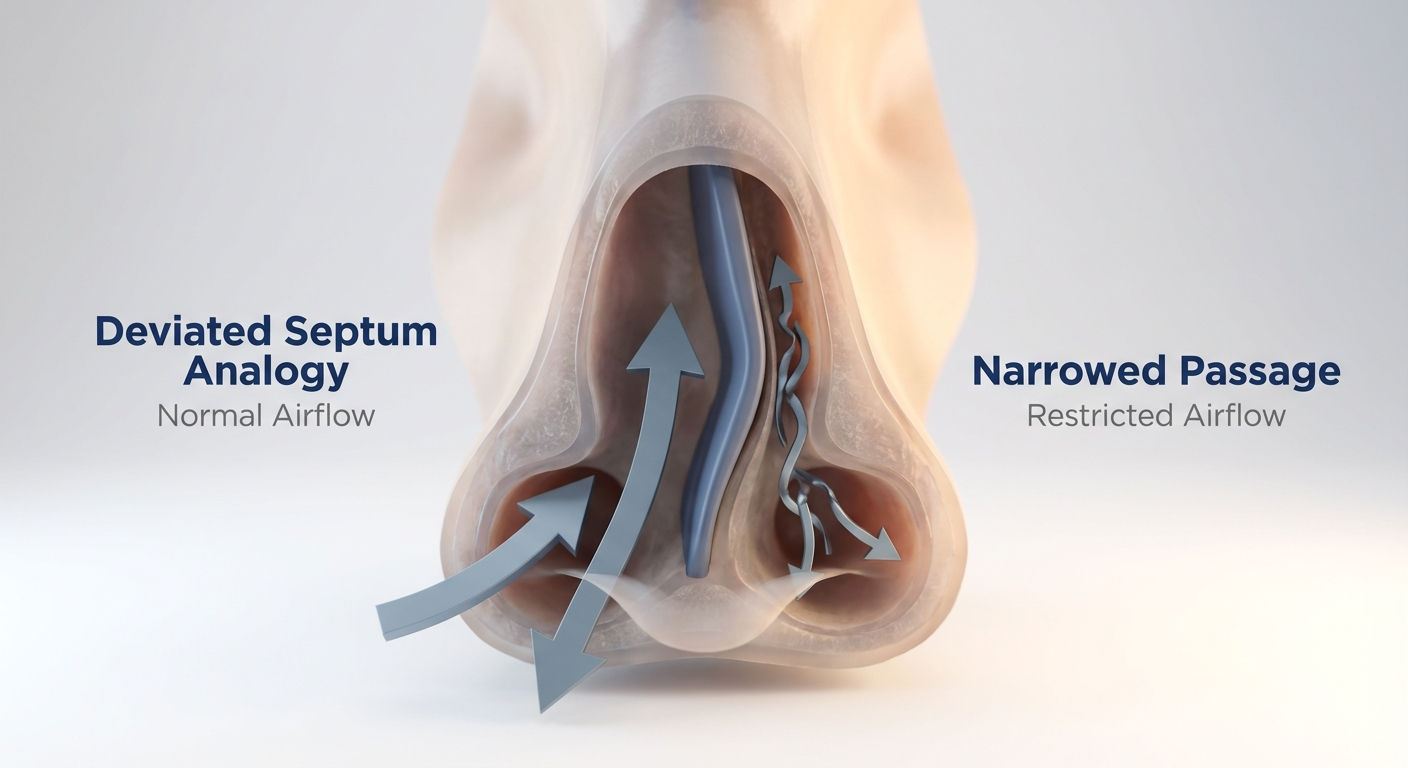
A helpful way to picture it: breathing through your nose can start to feel like trying to sip through a pinched straw—you can get some air, but it takes more effort, and it’s not comfortable.
You might also notice little workarounds: sleeping with your mouth open, turning your head to “find the better side,” or feeling like you can’t keep up during a workout because you never quite catch a full breath through your nose.²
Nasal obstruction vs. nasal congestion
People use these terms interchangeably, but they can point to different mechanisms:
• Nasal congestion often implies swollen, inflamed tissue, commonly from colds or allergies.¹²
• Obstruction can be structural, inflammatory, or both—and may not resolve on its own.¹²
A clinician might put it this way: “Congestion is often the swelling. Obstruction is the narrowing—from swelling, anatomy, or both.” If you’ve tried typical cold/allergy approaches and still feel stuck, it may be time to look beyond short-term congestion. For more on differentiating causes, see deviated septum vs. allergies (how to tell the difference): https://www.clearpathnasal.com/blog/deviated-septum-vs-allergies-how-to-tell-the-difference
• It’s not just a nuisance—persistent obstruction is different from a short-lived stuffy nose and often needs a tailored plan.

Why Nasal Obstruction Matters More Than You Think
Sleep disruption and fatigue (a common hidden driver)
When nasal airflow is limited, sleep can suffer. Difficulty breathing comfortably through the nose may contribute to poor sleep quality and daytime fatigue.¹² Some people also notice more snoring or symptoms that overlap with sleep-disordered breathing—worth discussing with a clinician if sleep is consistently unrefreshing.
It’s also common for people to underestimate the sleep impact because it can be gradual. A typical pattern is: “I didn’t realize how tired I was until I had a few nights of better breathing.” For a deeper dive, see the link between nasal breathing and sleep quality: https://www.clearpathnasal.com/blog/the-crucial-link-between-nasal-airflow-and-quality-sleep-how-clearpath-nasal-balloon-offers-relief
Brain fog, focus issues, and productivity
Poor sleep plus persistent symptoms can add up. Over time, disrupted rest and chronic discomfort may negatively affect attention and cognitive performance.² In real life, that can look like feeling “wired but tired,” struggling to concentrate in meetings, or hitting an early-afternoon wall. While nasal obstruction isn’t the only cause of brain fog (hydration, stress, medications, and other conditions can also play a role), it can be a meaningful piece of the puzzle—especially when it’s paired with non-restorative sleep.²
Mental health impact: anxiety and depression risk
Living with chronic nasal obstruction (and the fatigue that can come with it) can take an emotional toll. Chronic nasal congestion/obstruction has been associated with worse mental health outcomes, including increased risk of anxiety and depression—often related to persistent symptoms and sleep disruption.³ This reflects association rather than direct causation, but symptom relief and better sleep can support overall well-being.³
• Better nasal airflow can support better sleep, energy, and day-to-day function—small improvements often add up meaningfully over time.

Common Causes of Nasal Obstruction (Structural vs. Inflammatory)
A practical way to think about causes is whether something is physically narrowing the airway (structural), swelling is reducing space inside the nose (inflammatory), or both.
Structural causes (something physically narrows the airway)
• Deviated septum (very common). Learn more: symptoms and treatment options for a deviated septum: https://www.clearpathnasal.com/blog/deviated-septum-explained-symptoms-causes-and-modern-treatment-options ²⁴
• Nasal valve collapse (narrowing/weakness at the nasal valve area)²
• Nasal polyps (soft, noncancerous growths that can block airflow)¹²
• Turbinate hypertrophy (enlarged turbinates that take up airflow space)²
Everyday example: structural issues can feel like a doorway that’s partly blocked by the frame—no matter how much you “reduce irritation,” the opening is still limited.
Inflammatory causes (swelling inside the nose)
• Allergic rhinitis (seasonal or year-round allergies)¹²
• Chronic rhinosinusitis / sinusitis²⁴
• Environmental irritants (smoke, strong odors) and medication overuse (rebound congestion from decongestant sprays)²
Inflammation is more like the doorway is technically wide enough—but the “walls” inside swell and reduce the space you have to breathe.
Often it’s both
A very common scenario: a deviated septum narrows one side, and then allergies cause turbinate swelling—making the narrowing feel much worse. Treating only one part of the problem can lead to incomplete relief.² For more on differentiating, see deviated septum vs. allergies: https://www.clearpathnasal.com/blog/deviated-septum-vs-allergies-how-to-tell-the-difference
• Many people have both structural and inflammatory drivers—addressing each piece usually works best.
Nasal Obstruction in Children: When to Look Beyond “Constant Congestion”
Kids can absolutely have persistent “stuffy nose” symptoms—but the cause is not always repeated colds.
Enlarged adenoids are a common cause
Enlarged adenoids can contribute to ongoing obstruction in children. Clues may include:
• Mouth breathing
• Snoring
• “Nasal” voice
• Restless sleep²
Parents often describe it as: “They always sound congested, even when they’re not sick.”
Why treatment matters for development and school
Untreated obstruction and poor sleep may contribute to behavioral concerns, daytime sleepiness, and reduced academic performance in some children.² Because kids are still developing, chronic poor sleep can also show up as irritability or trouble focusing—sometimes mistaken for “just a phase.”²
When parents should seek evaluation
Consider an evaluation if a child has:
• Persistent mouth breathing
• Nightly snoring
• Pauses in breathing
• Recurrent ear/sinus infections
• Daytime sleepiness²
• In kids, persistent obstruction and poor sleep deserve attention—evaluation can protect growth, behavior, and learning.

Symptoms That Suggest Your Blocked Nose Isn’t Just a Cold
Signs it may be chronic or structural
• One-sided blockage that doesn’t switch sides
• Symptoms that last more than 10–14 days repeatedly or are present most days²
• Mouth breathing, dry mouth
• Reduced smell
• Frequent sinus pressure/headaches¹
One practical rule of thumb: if you’re repeatedly asking, “Why does this never fully go away?” it’s worth considering a more complete evaluation.
Red flags—seek urgent medical care
Seek urgent care for:
• Significant nosebleeds
• High fever with severe facial swelling
• Vision changes
• Severe headache
• Symptoms after nasal/facial trauma¹
• If symptoms are persistent, one-sided, or severe, don’t wait—get evaluated promptly.
How Nasal Obstruction Is Diagnosed (What to Expect at an ENT Visit)
History + nasal exam
Clinicians typically ask about timing, triggers, whether symptoms are one-sided, allergy history, and medication use.² Helpful details to bring (or track for a week): what makes it worse (exercise, nighttime, pollen season), what you’ve tried (sprays, rinses, pills), and whether anything helps temporarily.
Nasal endoscopy (quick, in-office)
A nasal endoscopy can help identify issues like septal deviation, polyps, inflammation, or nasal valve concerns.² Many patients worry this will be painful. In practice, it’s typically brief, and clinicians often use topical medication to improve comfort.²
Imaging (only when needed)
CT scans may be used selectively—for example, if sinus disease is suspected or for surgical planning.²
• A focused history, simple in-office exam, and selective imaging usually reveal the main cause and best next steps.

Treatment Options: What Actually Helps Nasal Obstruction? (Step-by-Step)
The best plan depends on whether the driver is inflammation, structure, or both.
First-line medical therapy (when inflammation is part of the problem)
Common options include:
• Intranasal corticosteroids
• Antihistamines
• Saline irrigation¹²
A key point: consistent use matters. Some treatments may take days to weeks to reach full effect.² Also, avoid frequent or prolonged use of over-the-counter decongestant nasal sprays (for example, oxymetazoline or phenylephrine), which can cause rebound congestion if overused.²
Lifestyle and trigger control
Helpful strategies can include:
• Allergen reduction at home
• Humidification when air is very dry
• Avoiding smoke and strong irritants¹
These steps won’t change anatomy, but they can reduce the inflammatory “overlay” that often makes obstruction feel worse.
When procedures or surgery are considered
Procedural options may be discussed when:
• Symptoms persist despite optimized medical management, or
• There’s a clear structural cause (such as deviated septum, nasal valve collapse, or polyps).²
Procedures can include septoplasty and turbinate reduction, among others, depending on anatomy and findings.² The goal is not “a perfect-looking nose”—it’s more functional airflow and better day-to-day breathing.
• Matching treatment to the true driver(s)—inflammation, structure, or both—usually delivers the best relief.

Modern Septal Correction: Balloon-Assisted Endoscopic Septoplasty (Patient Overview)
One common structural cause of persistent symptoms is a deviated septum, which can create ongoing airflow limitation and mouth breathing.² For some patients, newer approaches aim to correct septal deviation with less tissue disruption. For a plain-language explainer, see: what is balloon septoplasty?: https://www.clearpathnasal.com/blog/what-is-balloon-septoplasty-a-minimally-invasive-option-for-deviated-septum
Why a deviated septum can cause real airflow limitation
When the septum is significantly off-center, it can narrow the nasal passage—sometimes mainly on one side—creating persistent obstruction that doesn’t respond well to allergy-only treatment.² A common pattern: “Allergy meds help a little, but that one side never truly opens.”
How balloon-assisted septoplasty is different (high level)
Balloon-assisted endoscopic septoplasty uses endoscopic visualization and directional hydrostatic pressure to mobilize the septum. In plain terms, it applies controlled fluid pressure inside a small balloon to gently reposition cartilage. A published retrospective analysis describes this approach as designed to reduce tissue disruption compared with traditional flap-based techniques.⁵ Discussion of specific devices, such as the ClearPath Nasal Balloon, is for informational purposes. Treatment decisions should always be personalized based on clinical evaluation.
What the ClearPath Nasal Balloon outcomes showed (key takeaways)
In a retrospective series of 107 cases using a force-directed balloon-assisted endoscopic septoplasty technique:
• Safety: No major intraoperative or postoperative complications were reported, including no septal perforation, hematoma, mucosal injury, or synechia.⁵
• Symptom improvement: Average 24% improvement in SNOT-22 scores at about 1 month, with notable relief in congestion and sleep-related complaints.⁵
• Imaging confirmation: In patients with pre/post CT scans (n=23), mean improvement in septal alignment was 45% at maximal deviation and 22% at the nasolacrimal duct (p=0.005).⁵
• Efficiency: The technique may reduce steps like flap elevation, suturing, and packing, potentially shortening anesthesia time.⁵
Results vary, and not all patients will experience the same outcomes. Retrospective studies are helpful but do not replace prospective, controlled data.⁵
Who might be a candidate (and who might not)
Potential candidates are patients with symptomatic septal deviation confirmed on exam. Not everyone is a fit—especially if symptoms are primarily inflammatory or if other anatomic factors change the best plan.² If you’re considering septal correction, it’s reasonable to ask your local ENT: “Am I a candidate for balloon-assisted septoplasty options like ClearPath, or would a traditional approach be better for my anatomy?”
• Talk with your ENT about whether a balloon-assisted or traditional septoplasty approach aligns with your anatomy, goals, and overall treatment plan.
FAQs Patients Ask About Chronic Nasal Obstruction
“Can allergies cause nasal obstruction?”
Yes. Allergies can cause swelling that reduces airflow, and structural issues can coexist.¹²
“Why is my nose blocked on one side?”
A normal nasal cycle can cause side-to-side changes, but persistent one-sided blockage can suggest a structural cause and should be evaluated.²
“Can nasal obstruction affect mental health?”
Chronic symptoms and poor sleep can worsen quality of life and are linked with higher risk of anxiety and depression.³
“When should I see an ENT?”
If symptoms persist, recur frequently, disrupt sleep, or don’t improve with appropriate medication, an evaluation is reasonable.²
• If your symptoms keep returning or never fully clear, an ENT can help identify the “why” and map a clear path forward.
When to Seek Help (and What to Do Next)
If nasal obstruction is affecting your sleep, work/school performance, exercise, or mood, it’s worth assessing the root cause. Many cases improve with a tailored plan that may include medication, lifestyle adjustments, and—when anatomy is a major driver—procedural options.¹² If you’ve dealt with “constant congestion” for weeks (or years), consider scheduling an evaluation with a local ENT. Bring a list of symptoms and what you’ve tried, and ask whether your obstruction appears inflammatory, structural, or both—and whether newer alternatives to traditional procedures, such as balloon-assisted septoplasty (for example, the ClearPath Nasal Balloon), are appropriate for you. Discussion of specific devices is provided for information only; decisions should be made with your clinician.
• You don’t have to live with chronic “stuffy nose”—effective, individualized options exist.
References
1. Cleveland Clinic. Nasal Obstruction. 2024. https://my.clevelandclinic.org/health/symptoms/nasal-obstruction
2. UpToDate. Nasal obstruction: Diagnosis and management. 2025. https://www.uptodate.com/contents/nasal-obstruction-diagnosis-and-management
3. Sleep and Sinus Centers. Chronic nasal congestion and its impact on mental health. 2026. https://sleepandsinuscenters.com/blog/chronic-nasal-congestion-and-its-impact-on-mental-health-what-you-need-to-know
4. Zadeh MD. What causes chronic nasal obstruction and how to treat it. 2023. https://www.zadehmd.com/post/what-causes-chronic-nasal-obstruction-and-how-to-treat-it
5. Dillard JD, Koudouovoh C, Lee V, et al. Outcomes of force-directed balloon-assisted endoscopic septoplasty: a retrospective analysis with a new technique and device. Rhinology Online. 2026;9:18–23. http://doi.org/10.4193/RHINOL/25.018
“This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.”
Resent posts
Contact us
Have questions about the ClearPath Nasal Balloon System? Our team is here to help with product inquiries, demonstrations, or order support.



.webp)